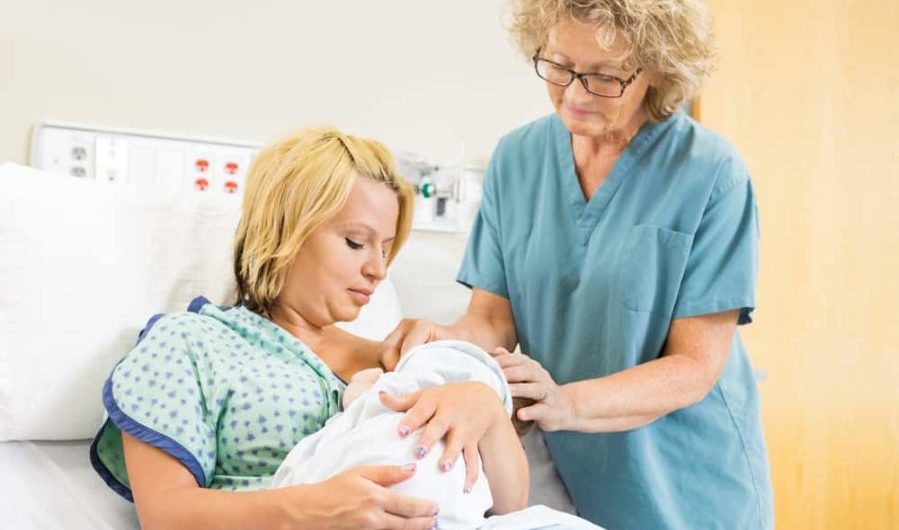
Building a Breastfeeding Support Plan
Below is a comment-question that we received on in response to our Pregnancy Calendar that we wanted to share here because we think others would benefit from the answer.
Medicaid runs out for me exactly 3 months after I give birth. So mine is a comment you’ve no doubt heard before, and it may not be appropriate. It is just that, “Definitely get a lactation specialist” on this Pregnancy Calendar entry is the kind of advice that I am unable to benefit from, and phrased as it is, it rather makes me feel like less of a good mother that I cannot.
Does that make sense? Or am I in the unreasonable throes of mid-pregnancy hormone-ry?
No, you’re right. That was an awfully inelegant way to phrase that advice, since it makes it sound like lactation support MUST BE some kind of specialty consultant you need to shell big bucks out for, like a private night nurse or infant sleep specialist. The good news is that it’s not!
Rely on Free Lactation Services at your Birthing Center
I certainly never hired a lactation specialist, but I leaned heavily on the lactation consultant services that were baked into my hospital’s maternity ward and pediatrician’s office. I know it can be super tricky to figure out exactly what Medicaid will cover (and so much depends on your state so I don’t want to get too deep into specifics here), but if you know where you’ll most likely be giving birth, call them. Ask them about what lactation support and services they offer — some maternity wards have a lactation specialist who will do rounds and check in on anyone trying to breastfeed; others have a specialist but will only dispatch them to you if you request it. Other times they’ll provide guidance in the form of a support group setting out in a common area.
At the very least, the Labor & Delivery nurses will all be able to help your baby to latch on correctly, show you a variety of breastfeeding positions, etc. This might be all you need! But the reason I gave the advice to seek out specialized breastfeeding support is simply because a lot of new moms do end up needing a bit more help than what they get from a day or two at the hospital, so it can be helpful to have someone to turn to after you’re discharged. And that someone can come from a wide variety of places.
Rely on Your Pediatrician’s Office for Lactation Advice
So next up, call your pediatrician’s office and ask if they have anyone on staff who can provide you with any lactation support or guidance while at your well-baby visits, if you find you need it. (Like say, your milk takes a while to come in, or you need a medicated nipple ointment, or you just plain aren’t sure if you’re getting a proper latch.) I would typically just put my baby on my boob in front of a nurse who would inspect the latch, mouth position, etc. and confirm that yay! He’s swallowing and getting milk, you’re doing fine.
Where to find Free Breastfeeding Support and Groups
THEN, look for free breastfeeding support groups or mother-to-mother “peer” support services.
1. According to WomensHealth.gov, your local WIC program may offer peer counselor services — meaning a mother who has successfully breastfed her own baby will be able to help you breastfeed your own. Here are some more resources on WIC breastfeeding support and services.
2. La Leche League International also has free groups all over the country to support breastfeeding mothers at all stages, from newborn to extended. (Though I recommend them with the caveat that they have a reputation for being a bit…pushy and breastfeeding-at-all-costs-even-if-it-really-isn’t-working-and-you’re-losing-your-mind. But that most likely varies wildly by group.)
3. Which…speaking of that. Do you know anyone who has successfully breastfed a baby? A trusted relative or close friend? Ask them if they wouldn’t mind stopping by the hospital or your home and check in on how you’re doing.
(Medicaid will also most likely cover a breast pump, so you can add that to your list of lactation prep to-dos. Pumps are a no-brainer if you hope to continue nursing while working, but also can come in handy in the very early days if you run into supply issues.)
ALL THIS SAID.
Final Thoughts
None of this has any bearing at all on whether you’re a “good” or “less good” of a mother. None of it! If you want to breastfeed, help and support are out there, but please don’t fall into the mental trap of breastfeeding = superior motherhood while formula = failure. Whether you breastfeed or not, get super great guidance or not, whether you have the ability to attend a support group or not — what matters is that you FEED YOUR BABY.
More Breastfeeding Advice from Alpha Mom:
1. Breastfeeding & 10 Things I Wish Somebody Had Told Me About It
2. Bottle Shame
3. Latch-22
Photo source: Depositphotos/Simplefoto

